Titanium vs Zirconia Abutments: Which Material Works Better for Implant Cases?
When dentists choose an implant abutment, the decision is not only about fit or workflow. Material selection also plays a major role in the final restorative result. Two of the main materials used today are titanium and zirconia, and each one offers distinct advantages depending on the clinical situation.
Some cases need maximum strength and long-term mechanical reliability. Other cases place more emphasis on esthetics, tissue appearance, and the visual transition from restoration to gingiva. This is why the question is not simply whether titanium or zirconia is “better” in general. The better choice depends on the case.
This page explains the real clinical differences between titanium and zirconia abutments, including strength, esthetics, tissue behavior, restorative indications, limitations, and how to choose the right option for different implant situations. Before choosing between titanium and zirconia, it’s important to understand the role of dental implant abutments in modern implant restorations.
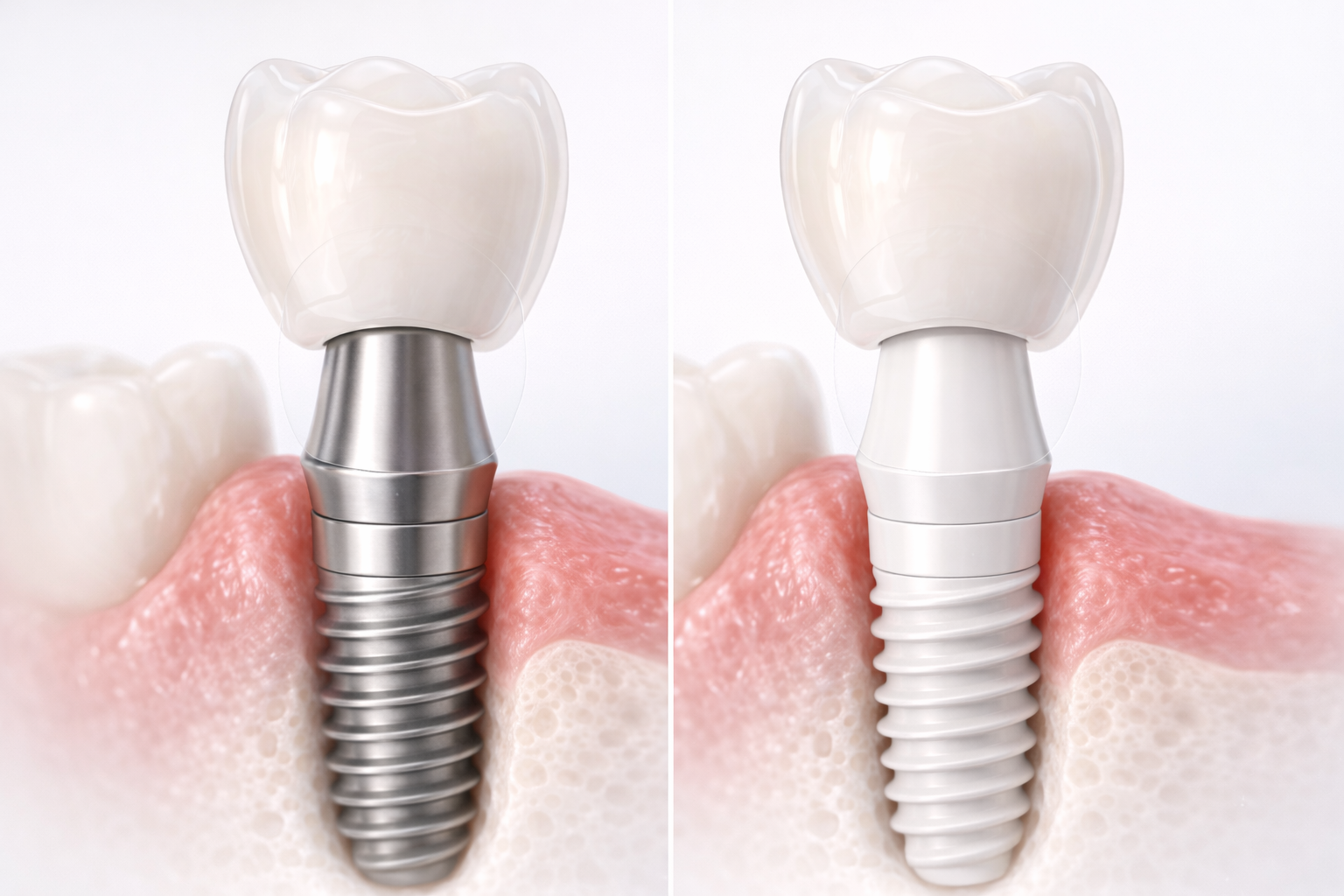
What Are Titanium and Zirconia Abutments?
Titanium abutments are implant abutments made from a strong metallic material that has long been used in implant dentistry because of its durability, corrosion resistance, and biocompatibility. Titanium is widely considered the standard material in many restorative workflows, especially when strength and mechanical predictability are the main priorities.
Zirconia abutments are made from a high-strength ceramic material that is tooth-colored rather than metallic. Their biggest advantage is esthetics. In many anterior cases, zirconia can provide a more natural visual effect under soft tissue and reduce the chance of gray shine-through, especially in thin gingival biotypes.
Both materials can be used successfully in implant prosthetics. The key is understanding where each material performs best and where each one may introduce limitations.
Why Material Choice Matters More Than It Seems
Abutment material affects more than just appearance. It can influence:
- the visual color under the tissue,
- how natural the cervical transition looks,
- how much strength the restoration has under load,
- the long-term behavior of the prosthetic connection,
- the restorative design options available,
- the suitability of the case for anterior or posterior use,
- how confident the dentist and lab can be in the final outcome.
This is why material selection should not be treated as a cosmetic afterthought. In many implant cases, especially visible ones, material choice becomes part of the restorative strategy from the very beginning.
Titanium Abutments: Main Strengths
Titanium remains the most common abutment material for good reason. It offers a combination of mechanical strength, reliability, and restorative versatility that is difficult to match.
One of the biggest advantages of titanium is strength under function. It performs especially well in posterior cases where chewing forces are higher and where the abutment may be exposed to greater long-term load. This makes titanium an excellent option for molars, premolars, and other force-dominant restorations.
Titanium is also highly familiar to both dentists and labs. It integrates easily into digital workflows, works well in custom CAD/CAM manufacturing, and is available across a wide range of implant systems and restorative designs.
In addition, titanium is often the safer choice when:
- implant angulation is challenging,
- restorative space is limited,
- occlusal load is high,
- the patient has parafunctional habits,
- the case requires maximum structural confidence.
For these reasons, titanium is still often considered the default material in many implant workflows.
Titanium Abutments: Main Limitations
Titanium does have limitations, especially in esthetic cases. Because it is metallic, it can sometimes influence the appearance of soft tissue, particularly in patients with thin gingiva. In highly visible areas, this may create a grayish visual effect or make the cervical area appear less natural.
This becomes more important in:
- anterior restorations,
- thin tissue biotypes,
- high smile line patients,
- cases where the gingival margin is highly visible,
- cases where the patient has strong esthetic expectations.
Titanium is not automatically a poor choice in the anterior zone, but it may require more careful restorative planning, especially if tissue thickness is limited.
Zirconia Abutments: Main Strengths
The greatest advantage of zirconia is esthetics. Because zirconia is tooth-colored, it can create a more natural appearance beneath the restoration and surrounding tissue. In anterior implant cases, this can be highly valuable.
Zirconia may help improve:
- visual tissue harmony,
- color transition at the cervical area,
- appearance under thin gingiva,
- esthetic perception in the smile zone,
- overall naturalness of the final restoration.
This makes zirconia especially attractive for single-unit anterior restorations where the goal is not only functional success but also a highly refined visual result.
Another important point is that zirconia works well in digitally designed custom abutment workflows. When the implant position is favorable and the case is properly selected, zirconia can be part of a very strong esthetic solution.
Zirconia Abutments: Main Limitations
Zirconia is not as universally forgiving as titanium in high-load situations. Even though it is a very strong ceramic, material behavior is different from metal. This means case selection matters more.
Potential limitations include:
- less confidence in high-force posterior situations,
- greater caution needed in bruxism cases,
- more sensitivity to design and thickness,
- less tolerance for poor implant positioning,
- greater need for carefully controlled restorative planning.
In many workflows, zirconia is used over a titanium base rather than as a purely one-piece ceramic abutment. This can help balance esthetics with mechanical stability, especially at the implant connection level.
When Titanium Makes More Sense
Titanium often makes more sense when function is the priority.
Examples include:
- posterior implant restorations,
- heavy occlusal load,
- bruxism or clenching risk,
- limited restorative space,
- non-ideal implant angulation,
- cases where maximum structural reliability matters more than cervical esthetics.
Titanium is also often preferred when the restorative team wants the most proven and predictable mechanical option. In simple terms, when strength and reliability dominate the decision, titanium is often the better choice.
When Zirconia Makes More Sense
Zirconia often makes more sense when esthetics are the priority.
This is especially true in:
- anterior single-tooth implant restorations,
- high smile line cases,
- thin gingival biotypes,
- patients with strong cosmetic expectations,
- situations where reducing metal show-through matters.
In these cases, zirconia may help create a more natural emergence and a cleaner cervical appearance. However, zirconia should still be selected carefully. It performs best when implant positioning, tissue support, and restorative design are already favorable.
Titanium vs Zirconia in the Esthetic Zone
In the anterior zone, achieving natural esthetics depends heavily on proper crown contour and soft tissue support. Tissue color, symmetry, contour, and emergence all affect whether the final case looks natural or artificial.
Titanium can still work in the anterior region, especially when:
- tissue is thick,
- the implant is ideally positioned,
- the crown design masks the substructure well,
- the patient does not show much gingiva when smiling.
Zirconia may offer an advantage when:
- tissue is thin,
- cervical translucency matters,
- gingival display is high,
- the restorative team wants to minimize metallic influence on tissue appearance.
This is why zirconia is often discussed as an esthetic material rather than simply an alternative material. Its value is strongest when visual softness and natural tissue integration matter most.
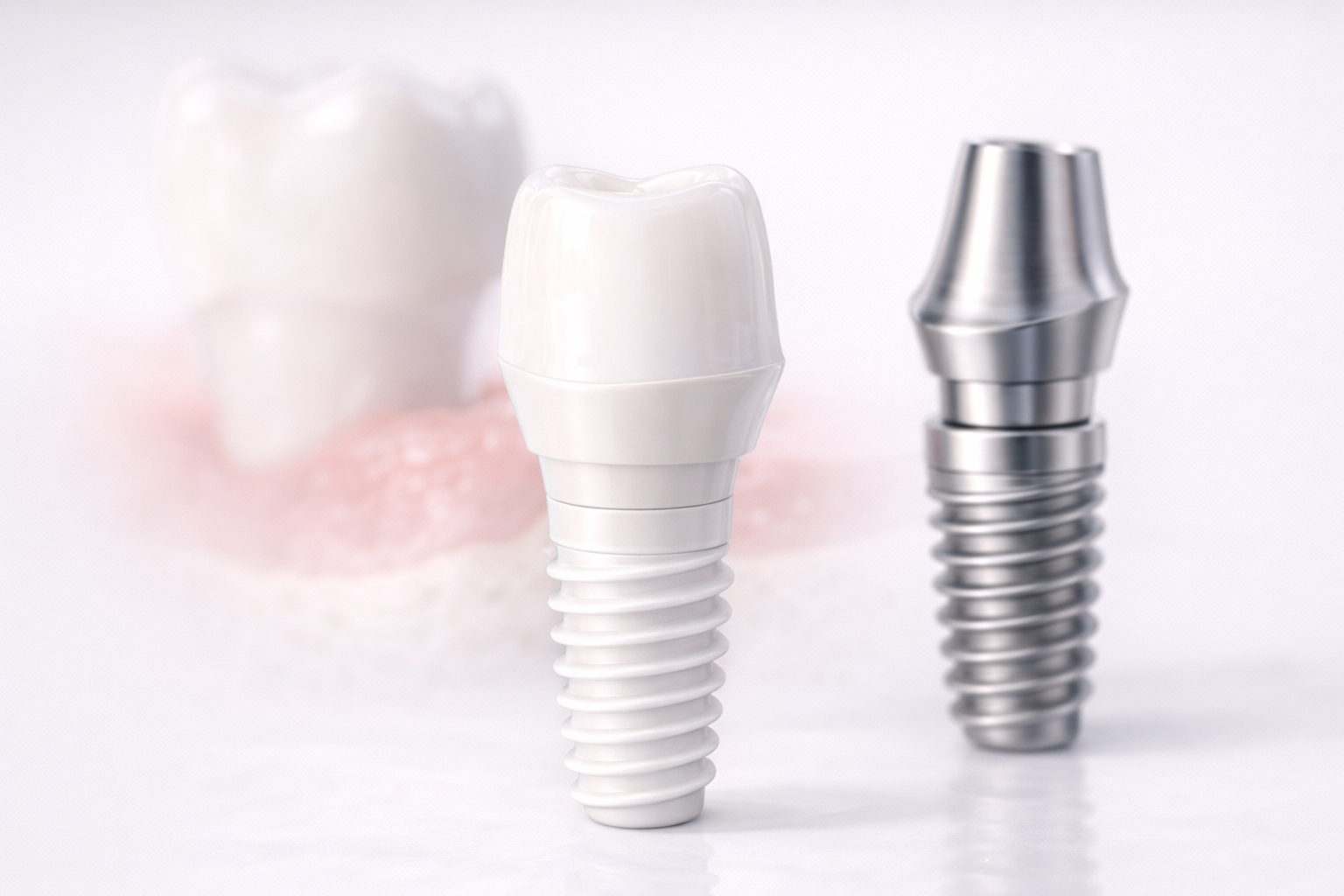
Titanium vs Zirconia in Posterior Cases
In posterior regions, material selection often depends on occlusal load and implant position. These are the situations where titanium often becomes the preferred option.
Molars and posterior premolars experience heavier chewing forces and often involve less esthetic pressure. In that environment, titanium offers practical advantages:
- greater confidence under load,
- broader restorative tolerance,
- less concern about visible substructure,
- strong long-term mechanical reliability.
Zirconia can still be used in selected posterior cases, but the threshold for case selection is higher. The more load, parafunction, or restorative complexity involved, the more titanium tends to make restorative sense.
The Role of Tissue Thickness
One of the biggest decision factors is soft tissue thickness. Thick tissue can often mask a metallic substructure well enough that titanium still looks acceptable even in relatively visible cases. Thin tissue, on the other hand, makes substructure choice more important.
In patients with a thin gingival biotype, the implant emergence profile becomes critical for achieving natural-looking results. When tissue is thin, zirconia may help reduce shine-through and improve the softness of the visual transition between restoration and gingiva. This does not automatically mean zirconia must always be chosen, but it does mean the esthetic consequences of titanium become more relevant.
In real clinical planning, tissue thickness often becomes one of the most practical filters in the titanium-versus-zirconia decision.
Digital Workflow and Material Planning
Today, material selection is increasingly influenced by the digital workflow. Modern digital workflows make it easier to choose and design the right abutment material for the case rather than using a one-material-fits-all approach.
With digital planning, the clinic and lab can evaluate:
- implant position,
- tissue contour,
- restorative space,
- emergence profile,
- smile zone visibility,
- crown material,
- the likely esthetic effect of the abutment underneath.
This makes material choice more intentional and more restorative-driven. Instead of deciding only from habit, the team can select the material based on the actual design needs of the restoration.
In many advanced workflows, this leads to better case matching:
- titanium for structurally demanding cases,
- zirconia for esthetic-sensitive cases,
- hybrid solutions when both priorities matter.
Common Mistakes in Material Selection
A common mistake is choosing zirconia only because it sounds more esthetic, without checking whether the case is truly favorable for ceramic-based restorative planning. If the implant is poorly positioned, load is high, or the case is functionally demanding, the esthetic benefit may not outweigh the structural concerns.
Another mistake is choosing titanium by default in every case, even when thin tissue and high smile line make esthetics more difficult. That may create a restoration that functions well but looks less natural than it could have.
A third mistake is ignoring the broader restorative design. Material should not be chosen in isolation. It should be selected together with implant position, crown material, tissue thickness, emergence profile, and the long-term maintenance plan.
How to Choose the Right Material
A practical approach is to ask a simple question first: is this case primarily strength-driven or esthetic-driven?
If the answer is strength-driven, titanium is often the leading option.
If the answer is esthetic-driven, zirconia may be more appropriate.
Then evaluate:
- anterior or posterior location,
- tissue thickness,
- smile line,
- implant angulation,
- restorative space,
- occlusal force,
- parafunctional risk,
- esthetic expectations,
- lab workflow and design confidence.
The best material is the one that supports the full restorative objective, not just one isolated feature.
Conclusion
Titanium and zirconia abutments are both valuable tools in implant dentistry, but they are not interchangeable in every situation. Titanium remains the stronger and more universally reliable choice in many posterior and force-dominant cases. Zirconia offers meaningful esthetic advantages in selected anterior and tissue-sensitive situations.
The right decision depends on what the case needs most. If function, load resistance, and structural predictability dominate, titanium often leads. If cervical esthetics, tissue appearance, and natural visual integration are the main priorities, zirconia may offer an advantage.
The best restorative outcomes usually come not from choosing one material by default, but from choosing the material that best matches the biology, mechanics, and esthetic goals of the case.
FAQ
What is the main difference between titanium and zirconia abutments?
The main difference is that titanium is a metallic material focused more on strength and structural reliability, while zirconia is a tooth-colored ceramic material often chosen for better esthetics.
Which material is better for posterior implant restorations?
Titanium is usually the better choice for posterior restorations because those cases place greater emphasis on strength and long-term mechanical stability.
Which material is better for anterior esthetic cases?
Zirconia is often preferred in anterior esthetic cases, especially when tissue is thin and the goal is to reduce metallic shine-through.
Can titanium still be used in the esthetic zone?
Yes. Titanium can still work well in the esthetic zone when tissue is thick, implant position is favorable, and the restorative design is carefully managed.
Is zirconia always more esthetic?
Not automatically. Zirconia often offers esthetic advantages, but only when the overall case design supports that benefit. Implant position, tissue thickness, and crown design still matter.
How should dentists choose between titanium and zirconia?
The decision should be based on location, tissue thickness, esthetic demand, occlusal load, implant position, and the restorative goals of the case.

