Custom Healing Abutments: How They Improve Soft Tissue Shaping Around Implants
Soft tissue management is one of the most important parts of implant restorative success. Even when implant placement is accurate and osseointegration is successful, the final result can still look compromised if the tissue around the implant is not shaped properly during healing. This is where healing abutments become highly important.
Standard healing abutments are widely used because they are simple and convenient. However, they create a generic tissue shape that does not always support the ideal emergence profile of the final restoration. In many implant cases, especially esthetic cases, this creates a gap between surgical healing and restorative planning.
Custom healing abutments help close that gap. Instead of forcing the tissue to heal around a standard round shape, they allow the tissue to heal around a form that is much closer to the intended final restoration. This can improve emergence profile, tissue contour, papilla support, and the overall transition from implant to crown.
This page explains what custom healing abutments are, how they differ from standard healing abutments, when they are most useful, and why they can make the final restorative phase more predictable. To fully understand their role, it’s important to look at how dental implant abutments function within the overall implant restoration process.
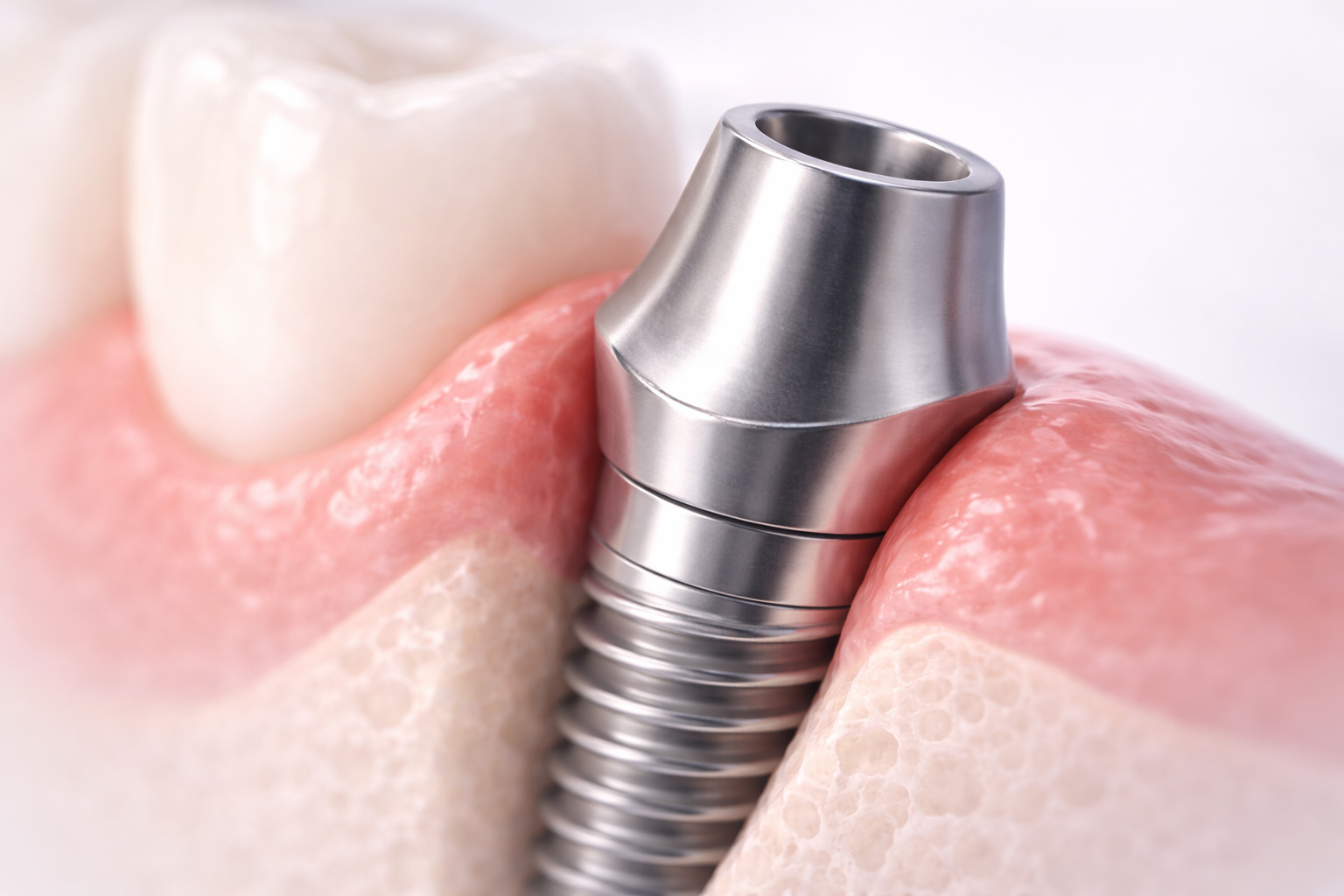
What Is a Healing Abutment?
A healing abutment is a temporary component connected to the implant during the healing phase. Its purpose is to help shape the soft tissue and create a transmucosal path between the implant and the oral environment.
In simple terms, the healing abutment helps guide how the gingiva heals around the implant. This matters because the shape of that tissue will influence the future restorative result. If the tissue heals in an ideal form, the final abutment and crown can often be placed more predictably. If the tissue heals in a generic or unfavorable form, the restorative team may later need to correct, reshape, or compensate for that tissue contour.
A standard healing abutment usually creates a round and simplified soft tissue opening. That may be acceptable in some posterior cases, but it often does not reflect the anatomy of the tooth that will ultimately be restored.
Why Soft Tissue Shaping Matters in Implant Dentistry
The soft tissue around an implant is not only a biological structure. It is also a major esthetic and restorative factor. Tissue contour influences:
- how natural the final restoration looks,
- how the crown emerges through the gingiva,
- how easy the area is to clean,
- how stable the papilla appears,
- how symmetrical the gingival architecture looks,
- how much the crown needs to compensate for tissue deficiencies.
If tissue is shaped poorly during healing, the final crown may need to be overcontoured to create the illusion of a natural emergence profile. That can make the restoration look bulky and become more difficult to maintain. It can also reduce the overall esthetic quality of the case.
This is why soft tissue shaping should not be treated as a secondary detail. In many cases, it is part of the restorative design from the beginning. Proper soft tissue formation depends heavily on the implant emergence profile, which determines how the restoration transitions from implant to crown.
What Makes a Custom Healing Abutment Different
A custom healing abutment is designed to support tissue healing in a patient-specific shape rather than a generic one. It is often fabricated based on a digital scan, the implant position, the planned crown form, or the extracted tooth anatomy.
Instead of creating a simple circular soft tissue tunnel, a custom healing abutment can support a more anatomical emergence profile. That means the tissue begins healing toward the shape needed for the final restoration rather than away from it.
This difference may sound small, but clinically it can be significant. A custom healing abutment can help:
- preserve tissue contour,
- support a more natural cervical form,
- reduce the need for later tissue conditioning,
- improve papilla development,
- make the transition to the final restoration smoother,
- reduce restorative compromise.
In many cases, the custom healing abutment acts as an early restorative tool, not just a healing component.
Standard Healing Abutments vs Custom Healing Abutments
Standard healing abutments are popular because they are simple, fast, and easy to place. They are often sufficient when:
- the case is posterior,
- esthetic demands are limited,
- tissue management is less critical,
- the final restoration does not require high tissue precision,
- the clinician wants a very straightforward surgical workflow.
Their limitation is that they are generic. They do not account for:
- tooth shape,
- emergence profile needs,
- tissue asymmetry,
- papilla goals,
- restorative contour,
- cervical architecture.
Custom healing abutments are more useful when:
- the case is in the esthetic zone, tissue shape matters,
- the patient has a high smile line,
- a natural emergence profile is important,
- the final restoration needs a more anatomical tissue form,
- the team wants to reduce later tissue correction.
The advantages of customization become more evident when evaluating stock vs custom abutments in terms of tissue adaptation and precision. This is why custom healing abutments are not simply “better” in every case. They are more strategic. Their value becomes strongest when tissue contour plays a visible and restorative role.
Why Custom Healing Abutments Can Improve the Final Restoration
The final restoration always depends on what the soft tissue allows. If the tissue has collapsed, healed flat, or formed a shape that does not support the intended crown, the restorative team has fewer options.
Custom healing abutments can improve the final restoration by improving the tissue conditions before the final abutment and crown are even placed.
This may lead to:
- a more natural emergence profile,
- better cervical contour,
- less overcontouring,
- smoother tissue adaptation,
- improved papilla support,
- less need for prolonged provisional shaping,
- a more efficient restorative phase.
In other words, a custom healing abutment helps create better starting conditions for the definitive restoration. Instead of asking the crown or final abutment to solve every tissue problem later, the tissue is shaped earlier and more intentionally.
When Custom Healing Abutments Make the Most Sense
Custom healing abutments are especially useful in cases where tissue shape strongly affects the esthetic and restorative result.
Examples include:
- anterior single-tooth implants,
- high smile line cases,
- thin gingival biotypes,
- immediate implant placement,
- cases where tissue collapse is a concern,
- situations where papilla preservation matters,
- cases where the extracted tooth contour should be preserved as much as possible,
- restorations where emergence profile is a major priority.
They may also be very useful when the clinician wants to reduce the need for long tissue conditioning with provisional restorations later in the workflow.
In posterior cases, a custom healing abutment may still be helpful, but the value is usually lower unless tissue architecture remains important for restorative reasons.
Custom Healing Abutments in Immediate Implant Cases
Immediate implant cases are one of the strongest indications for custom healing abutments. When a tooth is extracted and an implant is placed immediately, the tissue is particularly vulnerable to collapse and contour loss.
In these cases, a standard healing abutment may not adequately support the existing tissue form. A custom healing abutment, by contrast, can be designed to reflect the shape needed to maintain the peri-implant tissue architecture more effectively.
This can be especially useful for:
- preserving the socket contour,
- supporting the cervical form,
- maintaining soft tissue profile,
- minimizing flattening of the tissue during healing,
- improving the esthetic starting point for the final restoration.
Immediate implants in the anterior zone are often where custom healing abutments show their greatest practical value.
How Custom Healing Abutments Relate to Emergence Profile
The implant emergence profile is the way the restoration rises from the implant platform through the gingiva into visible crown form. It is one of the most important visual and functional features of an implant restoration.
A custom healing abutment helps shape the tissue toward the emergence profile needed later. This does not mean it automatically creates the final shape on its own, but it gives the restorative team a much better foundation.
Without good tissue shaping, the final crown may need to create an artificial emergence. That usually means more bulk, less natural contour, and more plaque retention risk.
With better early tissue shaping, the final restoration can often be designed more cleanly and more naturally.
Custom Healing Abutments and Provisional Restorations
Some clinicians use provisional restorations to shape soft tissue over time. This can work very well, especially in advanced esthetic workflows. However, provisional shaping often requires additional appointments, adjustments, and time.
A custom healing abutment does not replace every provisional strategy, but it can reduce the amount of tissue correction needed later. In some workflows, it acts as an earlier and simpler stage of tissue conditioning.
This can make the provisional phase easier by:
- preserving more of the desired contour from the beginning,
- reducing tissue collapse,
- minimizing the amount of cervical reshaping needed later,
- allowing the restorative team to work from a more favorable tissue form.
In some cases, this leads to a more efficient restorative sequence and a smoother path to the definitive crown.
Materials Used for Custom Healing Abutments
Custom healing abutments are often fabricated from temporary or semi-temporary materials that are suitable for healing and tissue support. Common materials include:
- PEEK,
- PMMA,
- composite-based modifications,
- temporary abutment-based custom designs,
- digitally milled provisional materials.
The exact material depends on the workflow, the lab, the implant system, and the clinical goals of the case.
The most important factor is usually not the material alone, but whether the shape is appropriate for the tissue and restorative plan. A well-shaped custom healing abutment made through a good workflow often provides more value than a generic component made from a stronger but less adaptive material.
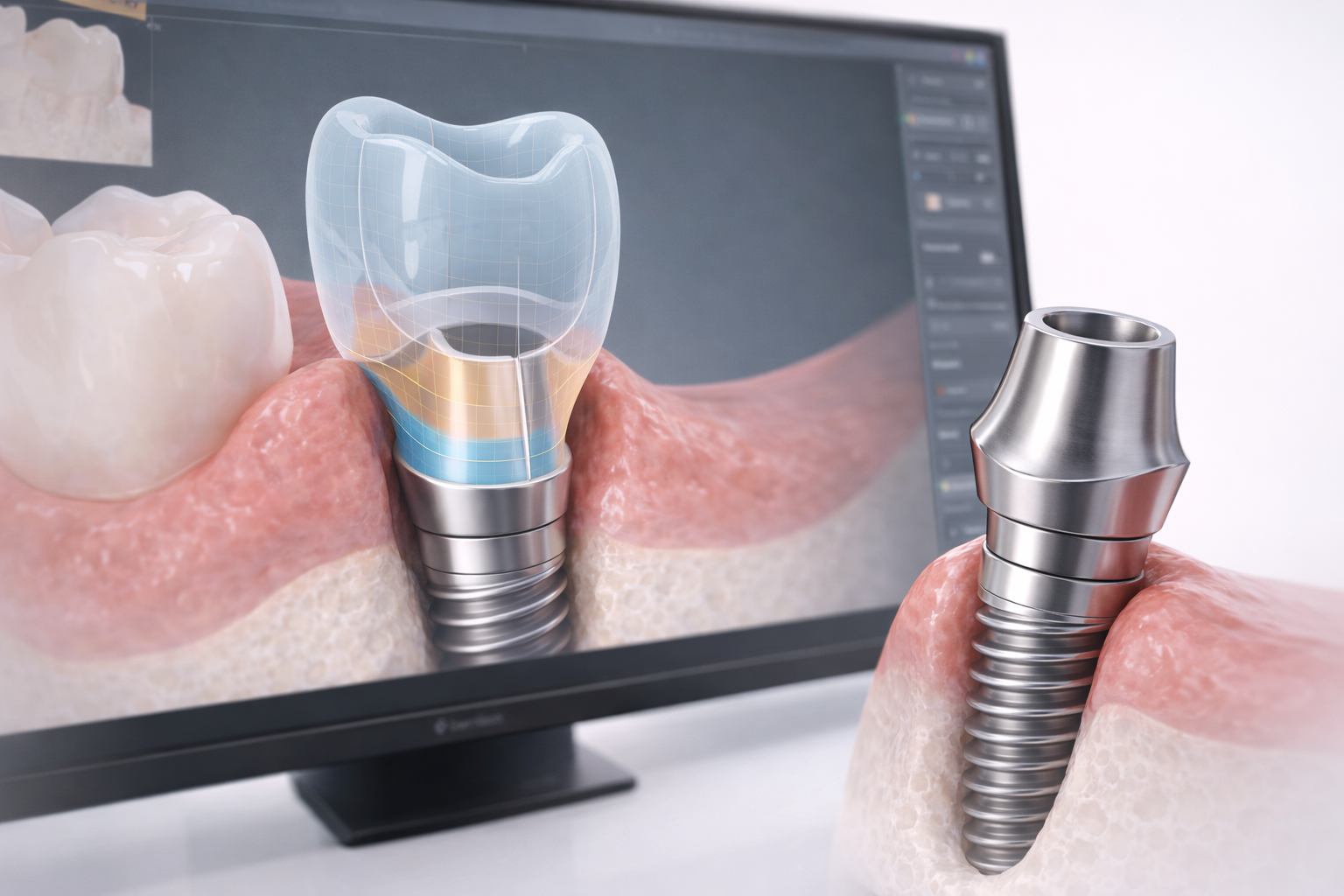
Digital Workflow for Custom Healing Abutments
Digital dentistry has made custom healing abutments much more practical than in the past. Instead of relying only on manual chairside modification, clinicians and labs can now use scan-based workflows to design patient-specific healing components.
A digital workflow may include:
- intraoral scanning,
- implant position capture,
- scan body alignment,
- digital tissue evaluation,
- CAD design of the healing contour,
- custom fabrication through milling or printing,
- lab-clinic communication before placement.
This makes the process more repeatable and often more precise. It also allows the healing component to be designed in relation to the future crown form rather than as a generic placeholder.
Today, many clinicians rely on the digital workflow for implant abutments to design customized healing solutions with greater precision. For modern implant workflows, this is one of the biggest reasons custom healing abutments are becoming more relevant. They fit naturally into digital planning and restorative-driven treatment design.
How the Lab Can Support Better Tissue Outcomes
The lab plays an important role in custom healing abutment success. A well-designed healing component depends on good communication and good case information.
For stronger outcomes, the lab should ideally receive:
- accurate digital scan data,
- implant system details,
- scan body information,
- photos of the soft tissue,
- information about the final restorative goal,
- esthetic priorities,
- notes about tissue preservation needs,
- immediate vs delayed placement context.
The more clearly the restorative goal is communicated, the better the healing abutment can support the tissue toward that goal.
Common Mistakes with Healing Abutment Planning
A common mistake is assuming that any healing abutment will do as long as the implant heals successfully. This ignores the restorative role of soft tissue architecture.
Another frequent mistake is waiting until the provisional or final crown stage to think seriously about tissue shape. By then, some of the lost contour may be harder to recover.
Other mistakes include:
- using standard healing components in highly esthetic cases without evaluating tissue consequences,
- failing to coordinate tissue shaping with the final crown plan,
- not communicating restorative goals to the lab,
- overlooking how immediate implant cases may need more anatomical tissue support,
- treating soft tissue form as cosmetic rather than restorative.
In many cases, better healing abutment planning does not add unnecessary complexity. It simply moves restorative thinking earlier in the workflow.
A Practical Way to Think About It
A simple question can help guide decision-making: does this tissue need to heal in a generic shape, or does it need to heal in a restoration-specific shape?
If the case is a straightforward posterior implant with low esthetic demand, a standard healing abutment may be entirely acceptable.
If the case is visible, tissue-sensitive, or emergence-driven, a custom healing abutment often makes more sense.
That decision should be based on:
- tooth location,
- tissue visibility,
- biotype,
- emergence needs,
- provisional strategy,
- final restorative expectations.
The more important the tissue architecture is to the final result, the more valuable custom healing becomes.
Conclusion
Custom healing abutments are valuable because they help shape tissue in a way that supports the intended final restoration rather than forcing the restoration to adapt to a generic healed form.
In routine cases, standard healing abutments may still be enough. But in esthetic, tissue-sensitive, or emergence-critical cases, a custom healing abutment often improves the starting conditions for the definitive result.
By supporting tissue contour earlier in the process, custom healing abutments can improve emergence profile, reduce restorative compromise, and make the final implant restoration more natural, more maintainable, and more predictable.
FAQ
What is a custom healing abutment?
A custom healing abutment is a patient-specific temporary component used during implant healing to shape the soft tissue in a way that better supports the future restoration.
How is a custom healing abutment different from a standard healing abutment?
A standard healing abutment creates a generic tissue opening, while a custom healing abutment is designed to support a more anatomical and restoration-specific tissue contour.
When are custom healing abutments most useful?
They are most useful in anterior cases, high smile line cases, immediate implant cases, thin tissue biotypes, and any situation where emergence profile and tissue contour matter.
Do custom healing abutments replace provisional restorations?
Not always. They do not replace every provisional workflow, but they can reduce how much tissue correction is needed later and make provisional shaping easier.
Why are custom healing abutments helpful in immediate implants?
They can help preserve socket contour and soft tissue architecture after extraction and immediate implant placement, especially in esthetic areas.
Can digital workflow improve custom healing abutment design?
Yes. Digital workflow makes it easier to design healing abutments based on implant position, tissue contour, and final restorative goals.

