Implant Crown Delivery Protocol for Dentists
Delivering an implant crown may appear straightforward, but the final restoration stage is one of the most critical phases of implant treatment. Even when implant placement and prosthetic design are correct, errors during crown delivery can compromise long-term success.
A structured delivery protocol helps clinicians ensure proper seating of the abutment, correct crown positioning, and complete removal of excess cement when necessary.
Following a consistent workflow significantly reduces the risk of complications such as crown instability, soft tissue inflammation, or peri-implant disease.
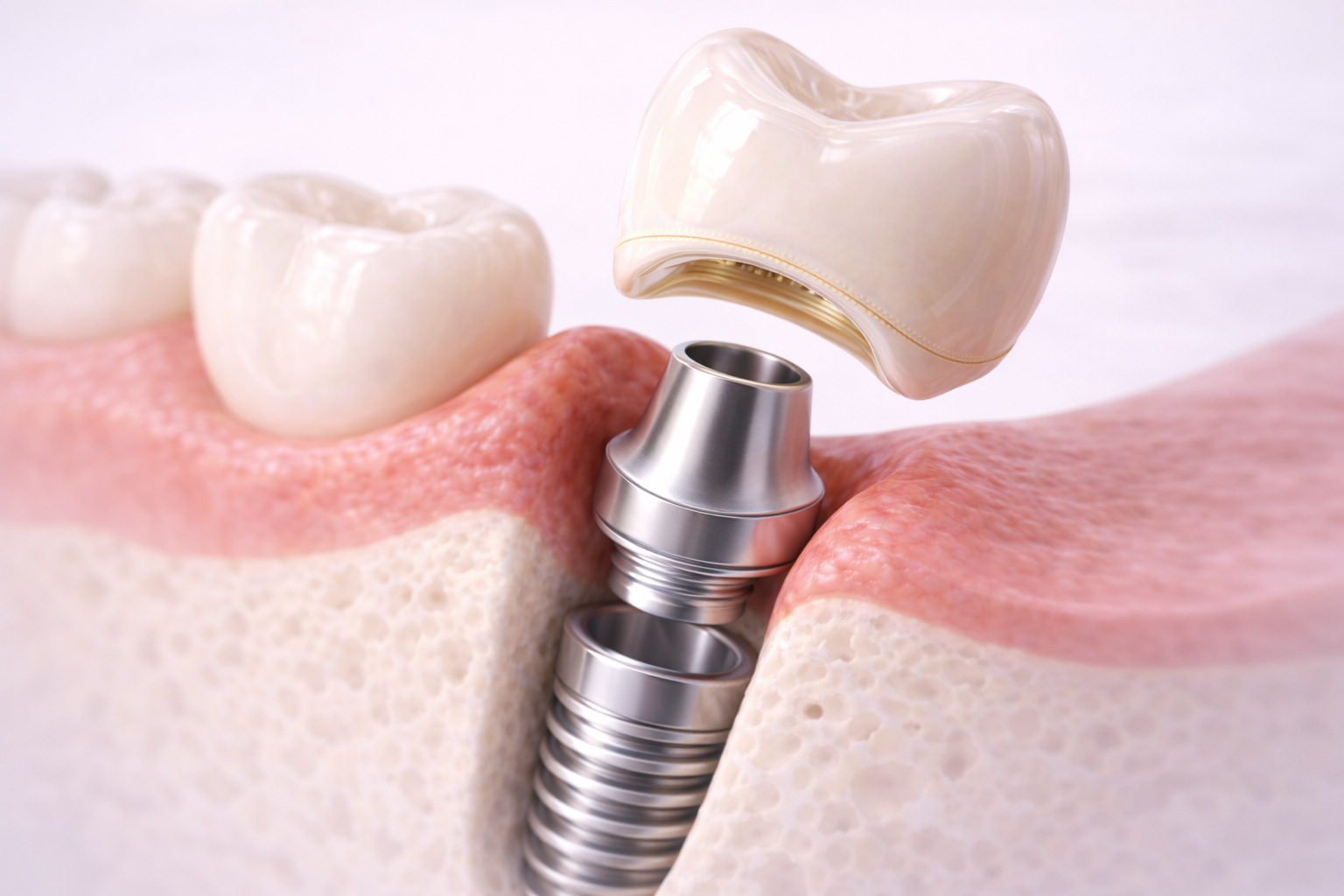
Step 1: Verify Implant and Abutment Seating
Before placing the crown, the clinician must confirm that the abutment is properly seated and tightened to the recommended torque.
Improper abutment seating can lead to misfit between the crown and abutment, which may result in occlusal problems or screw loosening.
The choice of abutment also plays an important role in crown delivery. Custom abutments often allow better crown seating and margin positioning.
You can read more about abutment selection in Stock vs Custom Abutments.
Step 2: Evaluate Implant Position and Restoration Design
Before the crown is delivered, clinicians should review how the implant position affects the final restoration.
Implants placed with unfavorable angulation may require adjustments in crown contour or abutment design to achieve proper occlusion and aesthetics.
Understanding the relationship between implant placement and prosthetic design is essential.
For more detail see How Implant Position Affects Abutment Choice.
Step 3: Check Crown Fit and Contact Points
Before final placement, the crown should be tested to confirm passive fit and correct interproximal contact.
The crown should seat fully on the abutment without rocking or resistance. Any resistance may indicate an internal misfit or debris inside the restoration.
At this stage clinicians also verify:
- proximal contacts
- occlusion
- crown contour
- emergence profile
The emergence profile plays an important role in soft tissue health and aesthetics.
To understand how emergence profile affects implant restorations, read Implant Emergence Profile.
Step 4: Manage Cement Carefully
When cement-retained restorations are used, cement management becomes one of the most important steps during crown delivery.
Excess cement left under the gingiva is one of the most common causes of peri-implant inflammation.
Clinicians should ensure that crown margins remain accessible for cement removal and that minimal cement is used during crown placement.
For a deeper explanation of margin placement see Abutment Margin Placement in Implant Restorations.
Another important decision is choosing between cement and screw retention.
You can read more about this in Screw-Retained vs Cement-Retained Restorations.
Step 5: Final Occlusion Check
After the crown is placed, clinicians should evaluate occlusion in both static and dynamic movements.
Implant restorations behave differently than natural teeth because implants do not have periodontal ligament support.
For this reason, occlusal forces should be carefully distributed to avoid overload.
Minor occlusal adjustments may be necessary to achieve optimal load distribution.
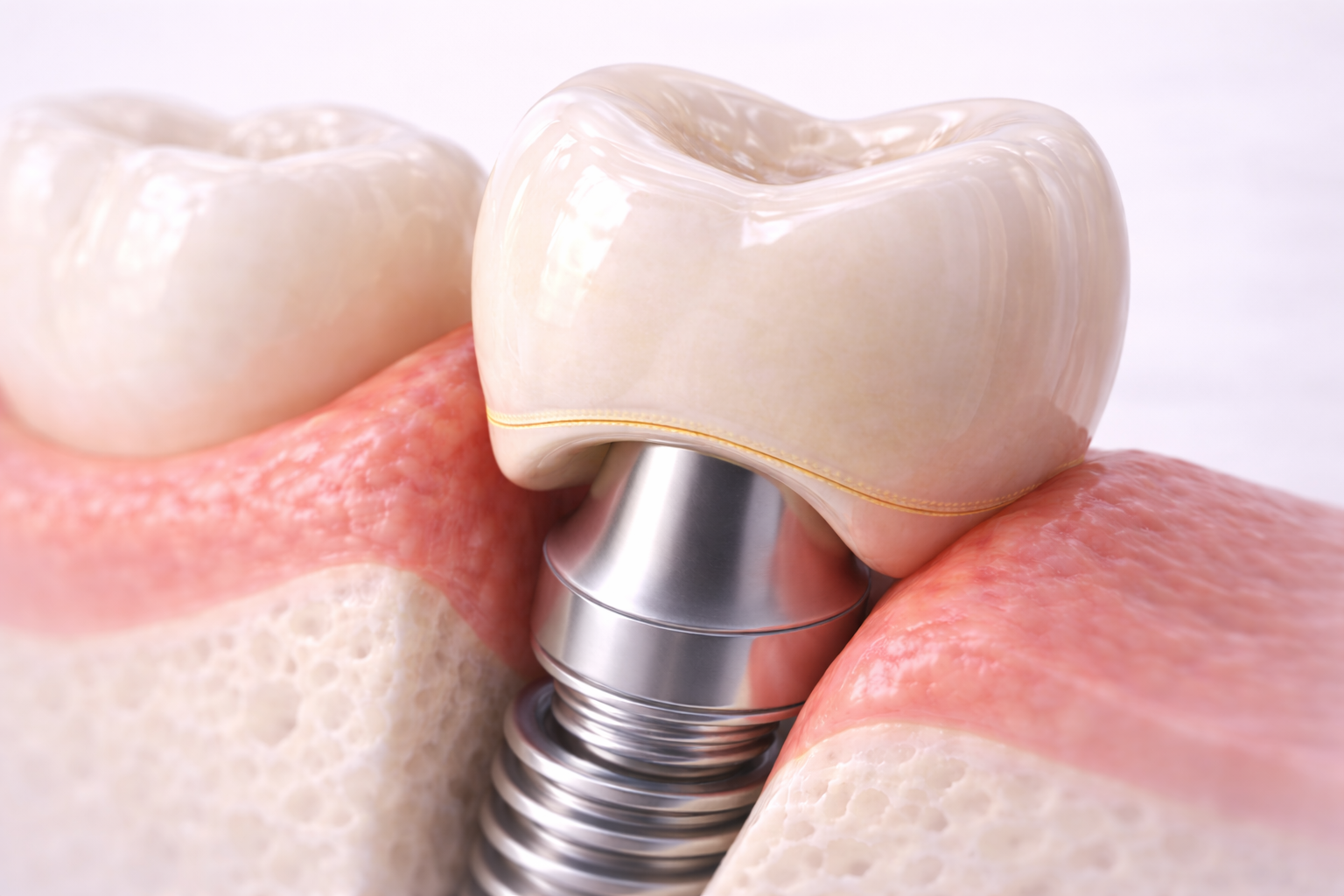
The Role of Digital Workflow in Crown Delivery
Digital planning tools are increasingly used to improve accuracy during implant restorations.
Digital workflows allow clinicians and laboratories to visualize crown design, emergence profile, and margin placement before the restoration is delivered.
This reduces the risk of misfit and improves communication between the clinic and the laboratory.
You can explore this topic further in Digital Workflow for Implant Abutments.
Conclusion
Implant crown delivery is a critical step that determines the final outcome of implant treatment.
By following a structured protocol that includes abutment verification, crown fit evaluation, careful cement control, and occlusal adjustment, clinicians can significantly reduce complications and improve long-term success.
Collaboration with the dental laboratory and proper planning remain essential elements of predictable implant restorations.

