Soft Tissue Management Around Dental Implants
Soft tissue management around dental implants plays a critical role in achieving predictable aesthetic and functional outcomes. Proper handling of peri-implant tissues helps shape the emergence profile, improves hygiene access, and supports long-term implant stability.
Healthy soft tissue supports the restoration, protects the implant interface, and contributes to both esthetic integration and long-term biological stability.
Without proper tissue management, even well-placed implants and well-designed prosthetics may encounter complications such as inflammation, plaque accumulation, and aesthetic inconsistencies.
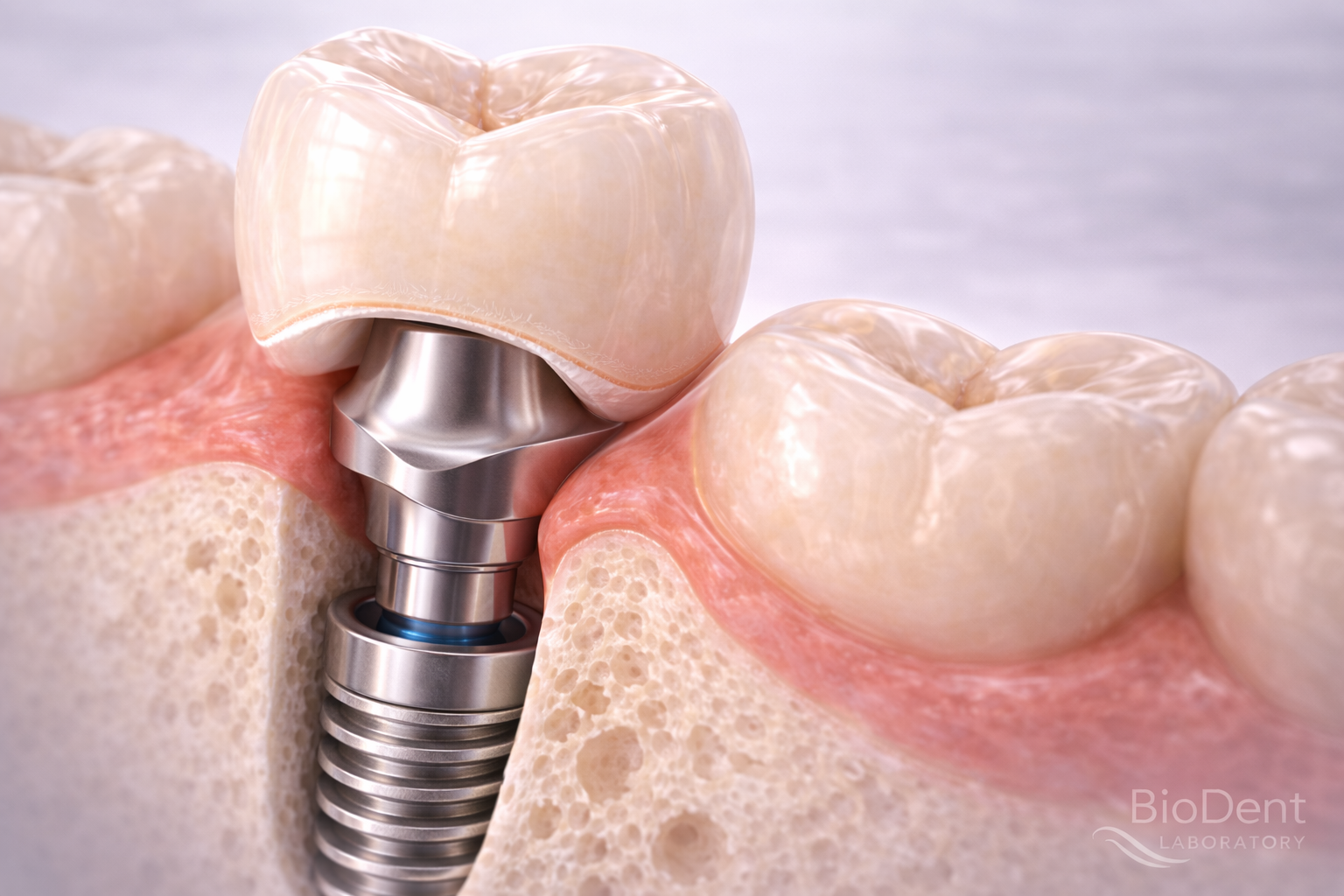
Why Soft Tissue Matters in Implant Restorations
Unlike natural teeth, implants do not have a periodontal ligament. This means that the surrounding tissue behaves differently and requires careful prosthetic and surgical planning.
Soft tissue around implants serves several important functions:
- protecting the implant platform
- supporting the emergence profile
- stabilizing gingival contours
- improving hygiene access
- contributing to esthetic integration
The shape and stability of soft tissue are influenced not only by surgery but also by the design of the prosthetic components.
One of the most important restorative factors affecting soft tissue is the emergence profile of the restoration.
For a deeper explanation see Implant Emergence Profile.
The Role of Emergence Profile in Tissue Stability
Emergence profile describes how the restoration transitions from the implant platform through the gingiva into the visible crown.
A well-designed emergence profile supports the natural contour of the gingiva and allows tissue to stabilize around the restoration.
When emergence profile is too abrupt or bulky, several problems may occur:
- tissue irritation
- plaque accumulation
- difficult hygiene
- unnatural gingival contour
Proper restorative design must guide soft tissue rather than compress or distort it.
To understand how crown contour affects tissue behavior, see Implant Crown Contour and Soft Tissue Support.
Custom Abutments and Tissue Support
Custom abutments often provide better control over soft tissue architecture than stock abutments.
By shaping the abutment specifically for the patient’s anatomy, clinicians and laboratories can create a more natural emergence profile and support gingival contours more effectively.
Custom abutments are especially helpful when:
- implant position requires restorative compensation
- tissue thickness varies across the site
- aesthetic contour must be controlled
- margin placement requires precision
For a deeper explanation of abutment design principles see Custom Abutment Design Principles in Modern Implant Dentistry.
The Role of Healing Abutments and Tissue Shaping
Soft tissue architecture begins forming long before the final crown is delivered.
Healing abutments and provisional restorations can help guide tissue development during the healing phase. By shaping tissue gradually, clinicians can create a more natural gingival contour before the final restoration is placed.
This approach often results in more predictable emergence profiles and better aesthetic outcomes.
To learn more about this process see Custom Healing Abutments.
Tissue Thickness and Implant Planning
Soft tissue thickness also influences restorative planning. Thin tissue biotypes may require more careful control of abutment design and crown contour to avoid visible metal or unnatural tissue contours.
In contrast, thicker tissue may provide more restorative flexibility but still requires careful management to prevent excessive bulk or plaque retention.
Implant position also influences tissue behavior and restorative possibilities.
For more on this relationship see How Implant Position Affects Abutment Choice.
Hygiene and Long-Term Tissue Health
Soft tissue health around implants depends heavily on the patient’s ability to clean the restoration.
Even beautifully designed restorations may fail if hygiene access is limited. For this reason, restorative contours should allow patients to clean around the implant with floss or interdental brushes.
Posterior implant restorations in particular must balance strength and hygiene accessibility.
To explore this topic further see Implant Abutments for Posterior Restorations.
Digital Workflow and Tissue Planning
Soft tissue management around dental implants is significantly enhanced by modern digital planning tools, allowing clinicians and laboratories to visualize soft tissue contours before the final restoration is produced.
Digital workflows make it possible to simulate the emergence profile, crown contour, and tissue support in advance. This enables clinicians to evaluate restorative options more precisely and optimize abutment design before fabrication, improving both functional and эстетические outcomes.
This collaborative approach improves communication and reduces restorative surprises during crown delivery.
For more information see Digital Workflow for Implant Abutments.
Conclusion
Soft tissue management is one of the most important aspects of implant dentistry. Healthy and stable gingival architecture contributes to both aesthetic outcomes and long-term implant success.
By combining careful surgical planning, thoughtful abutment design, and precise restorative contour, clinicians can create implant restorations that integrate naturally with surrounding tissue.
When soft tissue is properly supported and maintained, implant restorations become easier to clean, more comfortable for patients, and more predictable over time.

