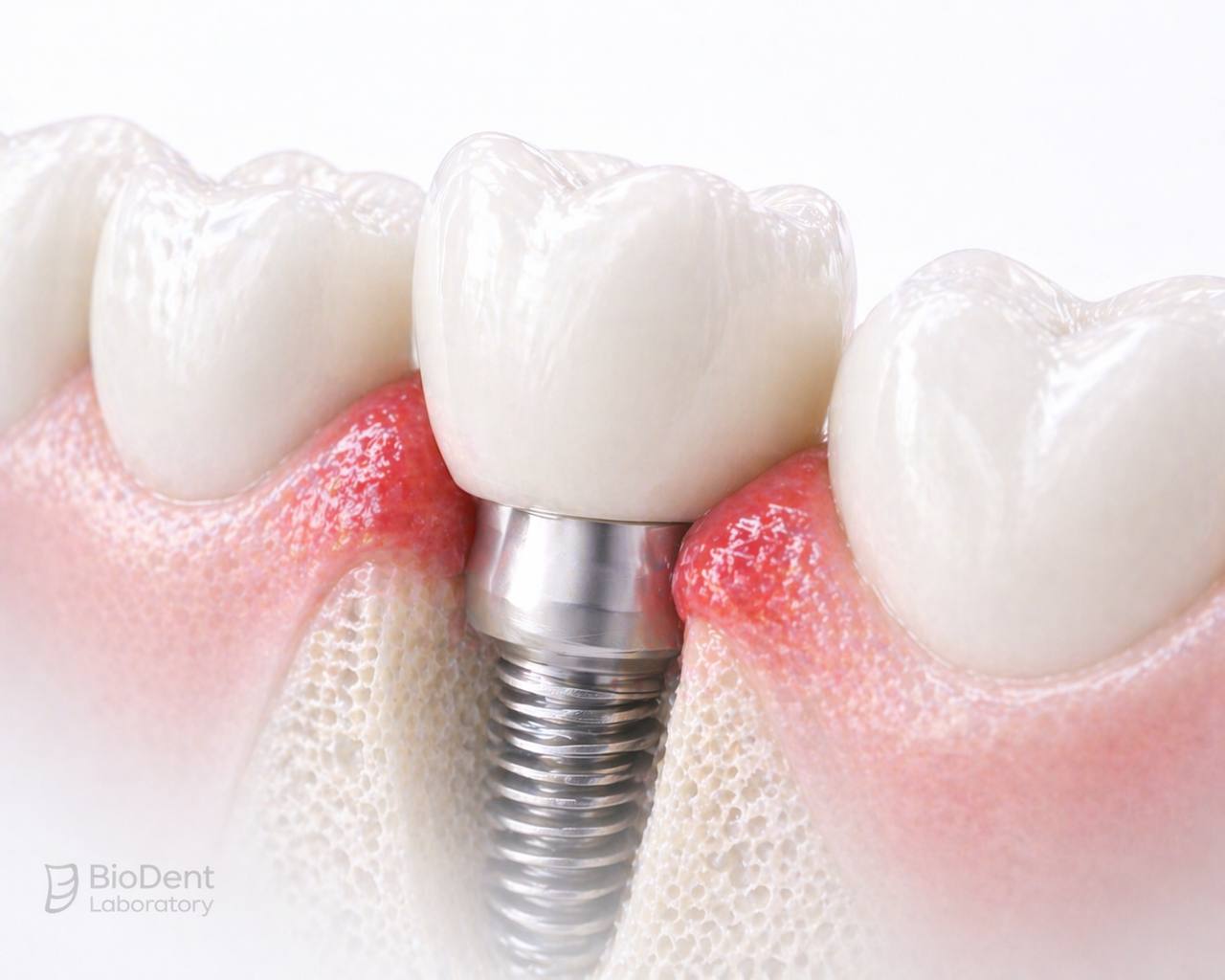
Peri-Implant Inflammation: Causes and Prevention
Peri-implant inflammation is one of the most common biological complications in implant dentistry. It often begins as mild tissue irritation but can progress into more serious conditions if the underlying cause is not identified and corrected.
In many cases, inflammation is not caused by a single mistake, but by a combination of restorative decisions. Crown contour, margin placement, cement control, implant position, and hygiene access all play a role in how soft tissue responds to an implant restoration.
Understanding these factors helps clinicians not only treat inflammation, but also prevent it at the planning stage.
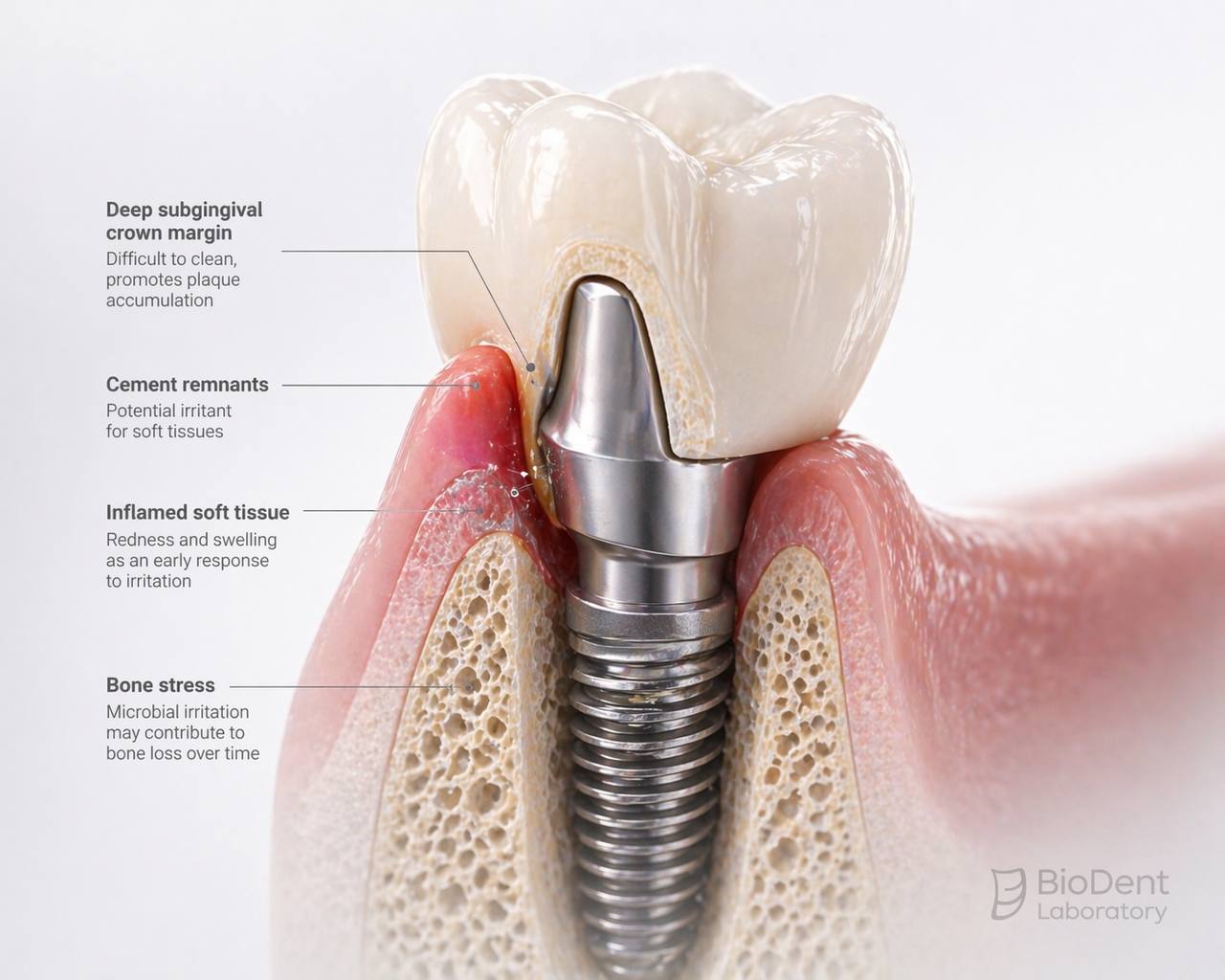
What Causes Peri-Implant Inflammation
Peri-implant inflammation typically develops when the tissue environment around the implant becomes difficult to maintain or biologically unstable.
Common causes include:
- residual cement
- over contoured crown design
- poor emergence profile
- deep subgingival margins
- limited hygiene access
- soft tissue compression
- plaque accumulation
- inadequate prosthetic planning
These factors often interact with each other rather than acting independently.
For a deeper understanding of one of the most critical causes, see Cement Removal Around Implant Crowns.
The Role of Crown Contour in Tissue Health
Crown contour has a direct impact on how soft tissue behaves around an implant restoration.
If the cervical area of the crown is too bulky, it can:
- trap plaque
- limit cleaning access
- create pressure on soft tissue
- disrupt natural tissue contour
Even when the crown looks esthetically acceptable, poor contour may still lead to long-term biological problems.
For more on this, see Implant Crown Contour and Soft Tissue Support.
Emergence Profile and Tissue Stability
Emergence profile determines how the crown transitions from the implant platform through the gingiva.
If the emergence profile is not properly designed, tissue may:
- become inflamed
- lose stability
- recede or swell
- trap plaque in inaccessible areas
A natural emergence profile helps support tissue rather than disturb it.
For more details, see Implant Emergence Profile.
Margin Placement and Cement Risk
Margin placement is one of the most critical factors in peri-implant inflammation.
Deep margins may:
- hide residual cement
- reduce visibility during cleanup
- increase difficulty of maintenance
- create long-term inflammation risk
This is why margin design must always consider both esthetics and accessibility.
For more on this, see Abutment Margin Placement in Implant Restorations.
Implant Position and Its Hidden Impact
Implant position influences almost every aspect of the restoration.
When the implant is placed too deep, too facial, or at an incorrect angle, the restoration may require compensation that negatively affects tissue health.
This can lead to:
- excessive crown bulk
- compromised emergence profile
- difficult margin access
- increased inflammation risk
For more on this relationship, see How Implant Position Affects Abutment Choice.
Hygiene Access Is Often the Real Problem
Many cases of peri-implant inflammation are not caused by the implant itself, but by the patient’s inability to clean around the restoration effectively.
This is often the result of:
- poor contour
- tight cervical areas
- inaccessible margins
- bulky posterior restorations
A restoration that cannot be cleaned is a long-term biological risk.
For more on posterior considerations, see Implant Abutments for Posterior Restorations.
Retention Strategy and Inflammation Risk
Retention method also plays a role.
Cement-retained restorations carry a higher risk of residual cement. Screw-retained restorations eliminate this issue but introduce other considerations such as access and angulation.
Choosing the correct retention strategy reduces biological complications.
For more on this, see Screw-Retained vs Cement-Retained Restorations.
The Role of Digital Workflow in Prevention
Digital workflow allows clinicians to plan:
- margin location
- crown contour
- emergence profile
- abutment design
- retention strategy
- before the restoration is fabricated.
This significantly reduces the risk of inflammation caused by poor design decisions.
For more on this, see Digital Workflow for Implant Abutments.
How to Prevent Peri-Implant Inflammation
Prevention begins with planning, not treatment.
Clinicians can reduce risk by:
- designing cleanable crown contours
- controlling emergence profile
- placing margins at accessible levels
- minimizing cement use
- selecting appropriate retention
- evaluating implant position early
- coordinating closely with the lab
These steps improve both short-term and long-term outcomes.
Conclusion
Peri-implant inflammation is rarely accidental. In most cases, it reflects how the restoration was planned and executed.
By understanding how abutment design, crown contour, margin placement, implant position, and hygiene access interact, clinicians can significantly reduce biological complications.
The most effective approach to inflammation is not only treatment — it is prevention through better prosthetic planning.
FAQ
What is the most common cause of peri-implant inflammation?
Residual cement and poor crown contour are among the most common causes.
Can crown design cause inflammation?
Yes. Over contoured crowns can trap plaque and limit hygiene access.
Does implant position affect inflammation risk?
Yes. Incorrect positioning often leads to restorative compromises that affect tissue health.
Is screw-retained restoration safer biologically?
It eliminates cement risk, which can reduce inflammation in many cases.
Can digital workflow help prevent inflammation?
Yes. It allows better planning of margins, contour, and abutment design.