Implant Crown Contour and Soft Tissue Support: Why Restorative Shape Matters
In implant dentistry, final esthetics are influenced by much more than implant placement alone. One of the most important restorative factors is crown contour — especially in the cervical and subgingival zones where the restoration interacts with the surrounding soft tissue. To better understand how esthetics and tissue stability are achieved, it’s important to consider the role of dental implant abutments in supporting the final restoration.
A crown can be technically well made and still produce a weak esthetic or biologic result if its contour does not support the tissue properly. This is one of the reasons implant restorations sometimes look bulky, artificial, difficult to clean, or unstable over time. In many of those situations, the real problem is not only the implant or the material. The problem is the restorative shape.
This page explains how implant crown contour affects soft tissue support, why contour design matters so much in implant prosthetics, and how dentists can create restorations that look more natural, support healthier tissue, and remain easier to maintain.
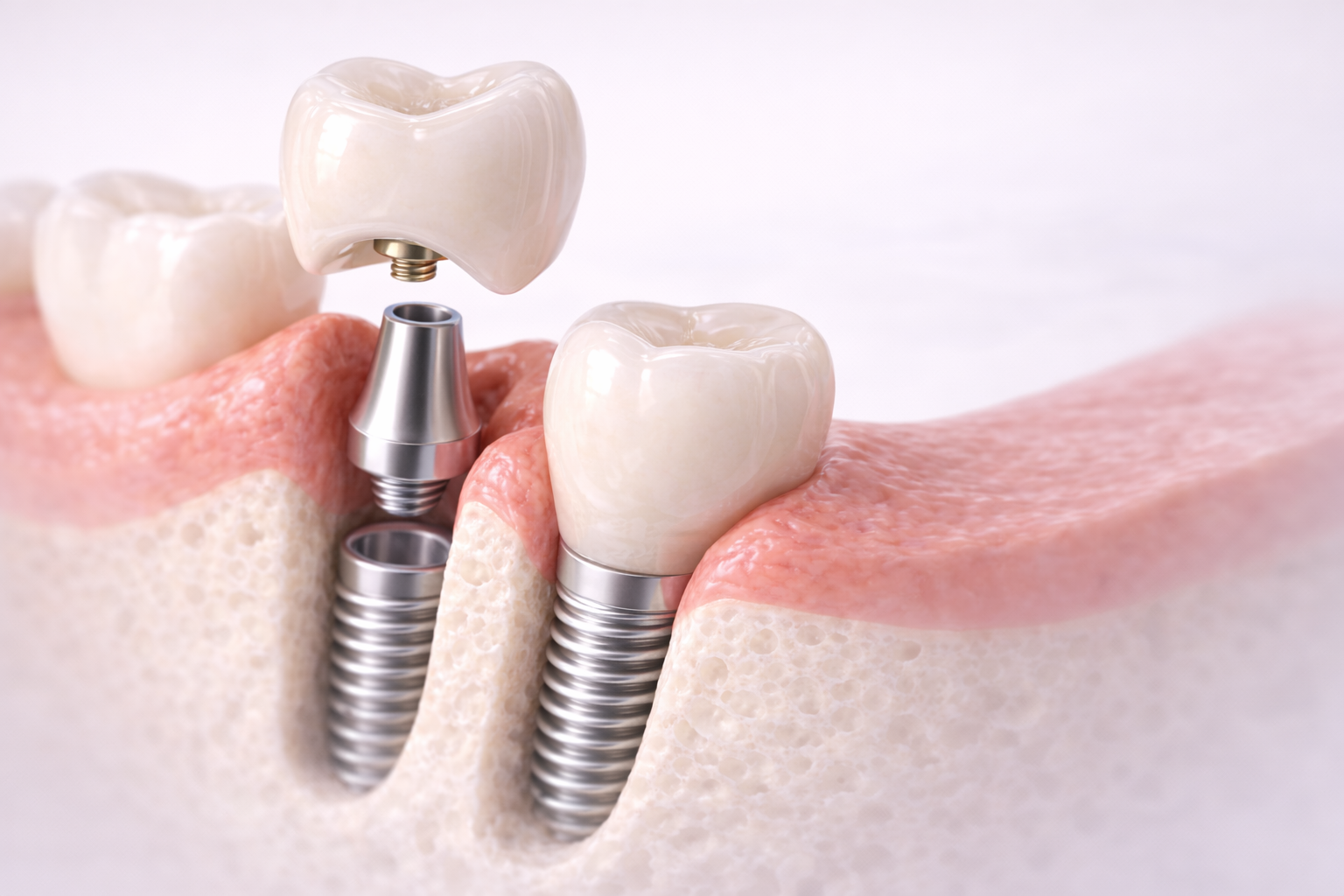
What Is Crown Contour in Implant Restorations?
Crown contour refers to the shape of the final restoration from the cervical zone upward into the visible crown form. The shape of the crown is closely related to how implant emergence profile is designed, as it defines the transition from implant to restoration. In implant prosthetics, this contour is especially important because the restoration must interact with soft tissue in a way that mimics natural anatomy without creating pressure, bulk, or plaque-retentive surfaces.
Unlike natural teeth, implants do not erupt through tissue with the same biologic relationship. That means restorative shape must do more work. The crown, together with the abutment, helps create the visual and functional transition between the implant platform and the visible tooth.
When contour is managed properly, the restoration can appear to emerge naturally from the tissue. When contour is poorly managed, the result may look overbuilt or prosthetic.
Why Crown Contour Matters More Than Many Dentists Expect
Crown contour affects several critical outcomes at the same time:
- soft tissue support
- esthetic transition from gingiva to crown
- papilla appearance
- plaque accumulation risk
- hygiene access
- emergence profile
- long-term tissue stability
- overall naturalness of the restoration
This is why crown contour is not simply a finishing detail. It is a major restorative design factor. In many implant cases, especially in the esthetic zone, contour determines whether the case looks refined or obviously artificial.
The Relationship Between Crown Contour and Soft Tissue Support
Soft tissue needs support, but it should not be forced into an unnatural shape. Soft tissue response is also influenced by the design of the abutment, especially when comparing titanium vs zirconia abutments. This balance is one of the most important principles in implant prosthetics.
If the crown contour is too flat, tissue may appear unsupported and the emergence may look weak or unnatural.
If the crown contour is too convex or bulky, tissue may become compressed, plaque control may become more difficult, and the final restoration may look overcontoured.
The goal is not maximum fullness. The goal is anatomical support. Crown contour should guide the tissue into a natural-looking form while preserving cleanability and biologic stability.
In practical terms, this means the restorative team must think carefully about the cervical third of the restoration, not just the visible incisal or occlusal anatomy.
Crown Contour and Emergence Profile
Crown contour and emergence profile are closely related, but they are not exactly the same thing.
Emergence profile describes the way the restoration transitions from the implant platform through the gingiva. Crown contour refers more broadly to the restorative form that continues beyond that emergence.
If emergence profile is the “exit path” from tissue, crown contour is the continuation of that shape into the visible tooth anatomy.
This is why crown contour must be consistent with the emergence profile. If the emergence is well designed but the crown becomes bulky immediately above the tissue, the result can still look unnatural. Achieving predictable results also depends on how implant position affects abutment choice in esthetic zones. Likewise, if the crown form is ideal but the emergence is poorly managed, the tissue relationship may still fail.
Why Overcontoured Implant Crowns Create Problems
Overcontouring is one of the most common restorative mistakes in implant cases.
It often happens when:
- implant position is less than ideal,
- the abutment is too generic,
- the restoration must compensate for facial implant placement,
- tissue support was not planned early enough,
- the final crown is asked to solve a problem that should have been solved at the abutment or healing stage.
An overcontoured crown may create several issues:
- bulky cervical anatomy,
- plaque retention,
- difficulty flossing or brushing,
- visual heaviness at the gingival margin,
- reduced tissue harmony,
- less natural emergence.
Even when the patient does not immediately identify the technical problem, they often perceive that the restoration looks less natural than a real tooth.
How Abutment Design Affects Crown Contour
The final crown contour is never determined by the crown alone. The abutment plays a major role.
If the abutment does not support the restoration properly, the crown may need to compensate with extra bulk. That is one of the main reasons custom abutments often improve contour outcomes.
A well-designed abutment can help:
- reduce cervical bulk,
- create cleaner emergence,
- support tissue more naturally,
- improve margin position,
- allow the crown to remain more anatomical.
A poorly chosen stock abutment may still work in simple cases, but in more demanding cases it can force the crown into less ideal contouring.
Soft Tissue Biotype Changes the Contour Strategy
Soft tissue biotype is a major factor in deciding how much contour support is appropriate.
Thin tissue biotypes are less forgiving. They may show restorative pressure, asymmetry, or recession more easily. In those cases, contour should usually be more carefully managed and often more conservative in how it supports the tissue.
Thick tissue is generally more stable, but even then, excessive crown fullness can still reduce hygiene access and make the restoration look heavy.
This means there is no universal contour formula. The correct shape depends on:
- tissue thickness,
- implant position,
- tooth location,
- esthetic risk,
- restorative material,
- final hygiene expectations.
Crown Contour in the Esthetic Zone
In anterior restorations, crown contour becomes one of the most visible and sensitive parts of the case.
Patients may not describe the issue in technical terms, but they often notice when the crown:
- looks too wide at the gumline,
- appears too round or too prosthetic,
- lacks natural cervical transition,
- disrupts the symmetry of the smile,
- creates a different gingival silhouette than the adjacent teeth.
This is why anterior implant restorations require a more refined contour strategy. The crown must support the tissue, but it must also respect the visual proportions of a natural tooth.
In these cases, contour design should be treated as part of the esthetic architecture of the smile.
Crown Contour in Posterior Implant Cases
Posterior cases usually reduce esthetic pressure, but contour still matters.
Even when the restoration is less visible, poor contour can still create:
- hygiene difficulty,
- food trapping,
- bulky cervical form,
- patient discomfort,
- long-term tissue irritation.
Posterior crowns often need to prioritize functional clearance, load distribution, and maintainability. That does not remove the need for good contour — it simply changes the reason why contour matters.
In posterior cases, the best contour is often the one that supports tissue adequately while remaining easy for the patient to clean.
How Custom Healing and Provisionals Influence Final Crown Contour
In many cases, optimal tissue shaping can be achieved with the use of custom healing abutments. It often begins during healing and provisionalization.
If the tissue is shaped well early in the workflow, the final crown can often be made more naturally and with fewer compensations. If the tissue collapses or heals in a generic form, the crown may later need to become bulkier to recreate missing support.
Custom healing abutments and provisional restorations can therefore improve final crown contour by improving the tissue architecture first.
This creates a better starting point for the definitive restoration.
Digital Workflow and Crown Contour Planning
Modern treatment planning increasingly relies on the digital workflow for implant abutments to achieve precise and predictable results.
With digital scans and CAD design, the clinic and lab can evaluate:
- tissue contour,
- implant angle,
- crown form,
- cervical emergence,
- restorative space,
- relationship to adjacent teeth.
This allows the restorative team to plan contour more intentionally rather than adjusting it only at the final stage.
In digital workflows, contour can be developed as part of a crown-driven design strategy. That means the abutment and crown are designed together with tissue support in mind.
This usually improves consistency and reduces restorative guesswork.
Contour and Hygiene Access
A beautiful implant crown that cannot be cleaned well is not a strong long-term restoration.
This is why contour must always be evaluated from the patient’s maintenance perspective. If the cervical zone becomes too convex or too bulky, hygiene around the implant becomes harder. Over time, that may increase plaque accumulation and soft tissue inflammation.
Well-designed contour should support both:
- natural esthetics,
- practical hygiene access.
This balance is one of the clearest signs of strong implant restorative planning.
Crown Contour and Retention Strategy
Retention strategy can also influence contour.
In screw-retained restorations, access channel position may affect restorative form. In cement-retained restorations, margin control and abutment contour may strongly influence how the final crown is shaped at the cervical zone.
This means contour should always be considered together with:
- abutment design,
- retention type,
- implant position,
- tissue conditions.
It is not an isolated decision.
Common Contour Mistakes in Implant Restorations
Several common mistakes reduce contour quality in implant cases:
- using the crown to compensate for poor implant position,
- ignoring tissue biotype,
- underestimating the cervical third of the restoration,
- creating too much facial fullness,
- designing for appearance without considering hygiene,
- failing to coordinate contour with abutment design,
- beginning contour planning too late in the workflow.
In many of these cases, the problem is not lack of technical skill. The problem is lack of early restorative planning around tissue and crown form.
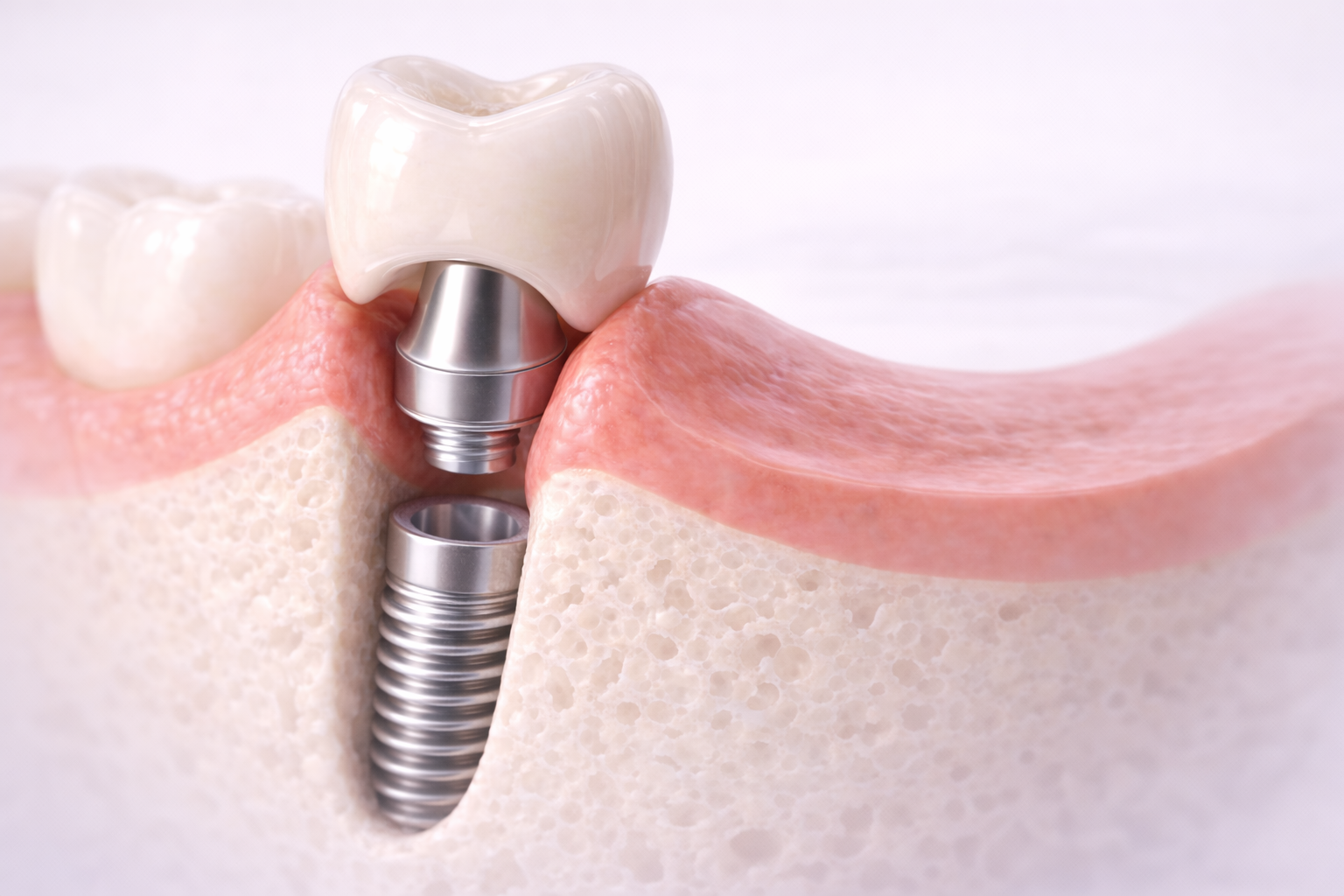
A Practical Clinical Approach
A useful question is this: does the crown contour support the tissue naturally, or is it forcing the tissue to adapt to a prosthetic compromise?
That question helps guide better decisions.
When planning contour, the clinician should evaluate:
- implant position,
- tissue thickness,
- crown width at the cervical zone,
- emergence profile,
- abutment shape,
- maintenance access,
- esthetic demands.
The best contour is not the fullest or the most dramatic. It is the one that supports healthy tissue and natural restorative form at the same time.
Conclusion
Implant crown contour is one of the most important restorative factors in determining whether a case looks natural, supports tissue properly, and remains maintainable over time.
When contour is planned well, the crown can support soft tissue without creating bulk or compromising hygiene. When contour is poorly planned, even a technically successful implant may produce an unnatural or biologically weak result.
The strongest outcomes usually come from planning crown contour early, in coordination with implant position, abutment design, tissue profile, and the final restorative objective.
FAQ
Why is crown contour important in implant restorations?
Crown contour affects soft tissue support, esthetics, emergence profile, hygiene access, and long-term tissue stability.
Can poor crown contour make an implant restoration look unnatural?
Yes. Overcontoured or poorly shaped cervical areas can make the restoration look bulky, artificial, and harder to clean.
How does abutment design affect crown contour?
Abutment design provides the foundation for the crown. A better abutment often allows a more natural crown contour with less restorative compromise.
Does soft tissue biotype change contour planning?
Yes. Thin tissue usually requires more refined and careful contour design than thicker tissue.
Can provisional restorations improve final contour outcomes?
Yes. Provisionals and custom healing components can help shape tissue earlier, creating better conditions for the final crown.
Why should crown contour be considered together with emergence profile?
Because the final restorative transition from implant to visible crown depends on both. They work together, not separately.

