Screw-Retained vs Cement-Retained Implant Restorations: How to Choose the Right Option
One of the most important decisions in implant prosthetics is whether the clinician should use a screw-retained or cement-retained restoration. Clinicians widely use both approaches. Both can work well. But they do not solve the same restorative problems in the same way.
The choice affects more than how the crown is attached. It influences retrievability, esthetics, maintenance, soft tissue risk, abutment design, implant angulation, restorative space, and long-term serviceability. In some cases, the difference is minor. In others, it can shape the entire restorative strategy from the beginning.
This page explains the real clinical differences between screw-retained and cement-retained implant restorations, when each option makes more sense, and how implant position, tissue conditions, and restorative priorities should influence the decision. When planning implant restorations, it’s important to understand how implant abutments function as the connection between the implant and the final prosthesis.
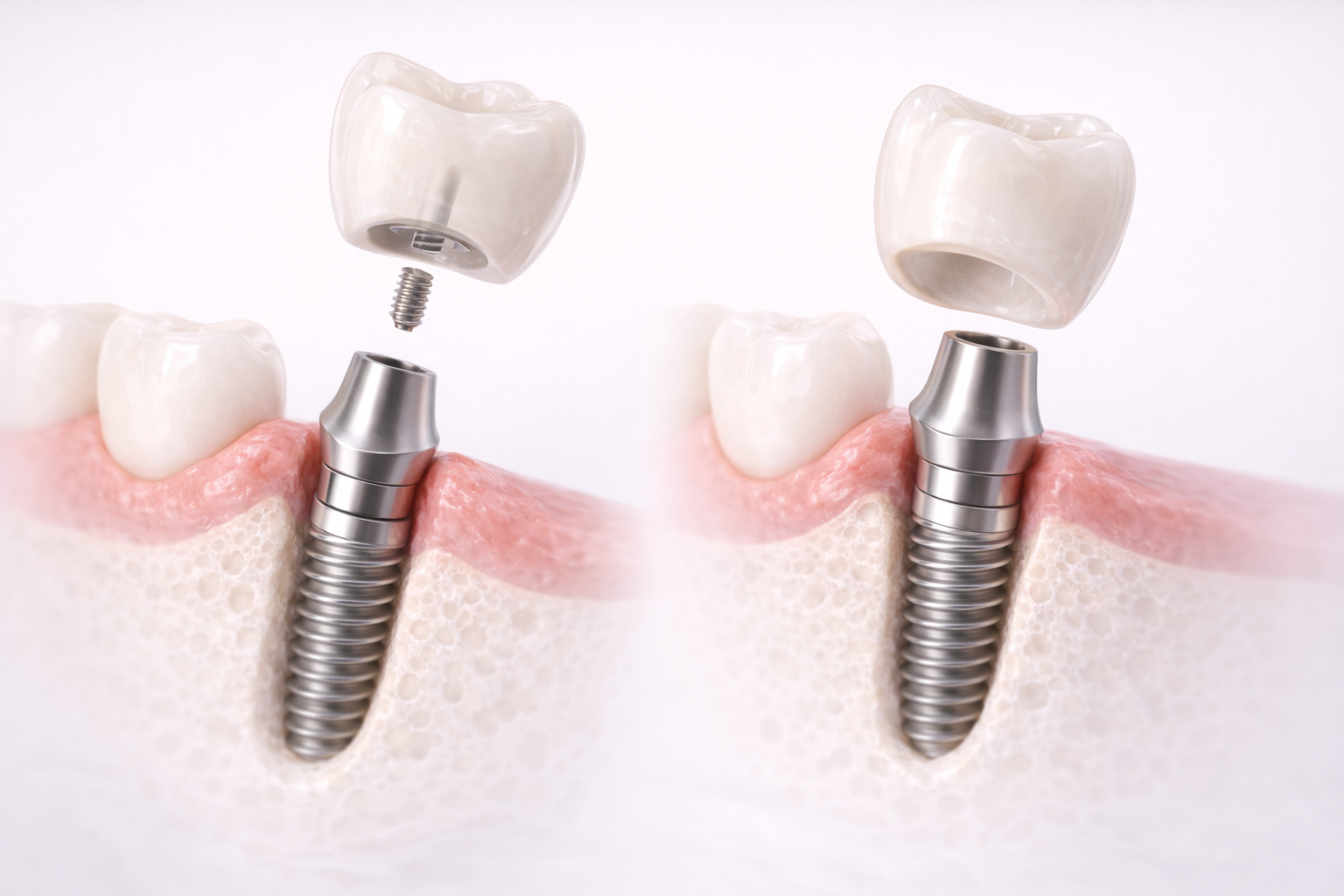
What Is a Screw-Retained Restoration?
A screw-retained implant restoration connects directly to the implant or to a screw-retained abutment using a prosthetic screw. It also includes a screw access channel, which clinicians later seal with a restorative material after final torque.
The biggest advantage of this design is retrievability. The crown or prosthesis can usually be removed more easily if maintenance, repair, screw tightening, hygiene intervention, or component replacement becomes necessary later.
This makes screw-retained solutions especially attractive in modern implant workflows where long-term serviceability is considered part of good restorative planning rather than an afterthought. The success of screw-retained restorations is closely related to how implant position affects abutment choice, particularly in terms of angulation and screw access.
What Is a Cement-Retained Restoration?
A cement-retained implant restoration is cemented onto an abutment rather than held in place by direct screw access through the crown. In this design, the abutment is first connected to the implant, and the crown is then cemented over it. This approach depends heavily on proper implant crown contour and soft tissue support to achieve optimal esthetic results.
The main advantage is restorative esthetics and flexibility. Because there is no visible screw access opening through the crown, the occlusal or facial surface may appear more natural in some situations. This can be especially attractive in cases where implant angulation would otherwise place the screw channel in an undesirable location.
However, cement-retained restorations introduce a different set of concerns, especially related to margin location and excess cement management.
Why the Decision Matters More Than It Seems
At first glance, the difference may appear technical. In reality, it influences several important restorative areas:
- how easily the restoration can be removed later,
- how the soft tissue is managed,
- how visible restorative compromises may be,
- how margins are designed,
- how likely cement-related complications become,
- how implant angulation affects the final result,
- how much flexibility the dentist and lab have in future maintenance.
This is why the retention decision should not be made only from habit. It should be made in response to the actual needs of the case.
The Biggest Advantage of Screw-Retained Restorations: Retrievability
The strongest argument for screw-retained restorations is retrievability.
If the clinician needs to:
- remove the crown,
- tighten a screw,
- inspect the implant-abutment connection,
- repair or replace a restoration,
- treat peri-implant issues,
- clean the prosthetic area more thoroughly,
- modify the restoration later,
- a screw-retained design usually makes this easier.
This is one of the main reasons many restorative teams prefer screw-retained restorations whenever implant position allows it. The ability to retrieve the restoration later can save time, reduce risk, and simplify long-term management.
In full-arch and more complex implant prosthetics, this advantage becomes even more significant. Modern solutions often rely on the digital workflow for implant abutments to improve precision and passive fit.
The Biggest Concern with Cement-Retained Restorations: Excess Cement
The biggest biologic concern with cement-retained restorations is residual cement.
If excess cement is left below the soft tissue margin, it may contribute to inflammation and create long-term complications around the implant. This risk becomes greater when margins are placed too deep or when implant depth and tissue thickness make cement cleanup difficult.
This does not mean cement-retained restorations are inherently wrong. It means they require more discipline in margin design, abutment planning, and cementation technique.
In well-managed cases with accessible margins, cement-retained restorations can work successfully. But if the case already presents depth, tissue, or visibility challenges, cement-related risk becomes more important.
When Screw-Retained Restorations Make More Sense
Screw-retained restorations often make more sense when:
- retrievability is a priority,
- implant angulation allows a favorable screw access path,
- the case may require maintenance later,
- the clinician wants to reduce cement-related risk,
- the restoration is full-arch or multi-unit,
- the patient presents higher biologic risk,
- long-term serviceability is important.
They are often especially useful in posterior cases and in cases where the screw access channel can emerge in an acceptable functional location.
As digital workflows continue to improve restorative precision, screw-retained solutions are increasingly viewed as a highly practical option rather than a compromise.
When Cement-Retained Restorations Make More Sense
Cement-retained restorations often make more sense when:
- implant angulation would create an undesirable screw access location,
- esthetics are highly sensitive,
- the clinician wants a more conventional crown form,
- the restoration is a single unit with manageable margin access,
- implant position supports a well-designed custom abutment,
- the case is carefully controlled and cement risk can be minimized.
In some anterior cases, a cement-retained restoration may help avoid a facial or incisal screw access issue that would reduce the visual quality of the crown. In those situations, cement retention may offer a more esthetic outcome, but only if margin design remains clinically manageable.
Implant Angulation Often Decides the Answer
In many cases, implant angulation is one of the strongest factors in the screw-retained versus cement-retained decision.
If the implant is ideally positioned, screw-retained restoration may be the most practical and maintenance-friendly choice.
If the implant angle causes the screw channel to emerge through an incisal edge, facial surface, or another undesirable location, the restorative team may need to consider other options:
- angulated screw channel concepts,
- custom abutment solutions,
- cement-retained design,
- different restorative planning to recover esthetics.
This is why the retention decision is rarely separate from implant position. Often, it is implant position that determines which option remains most reasonable.
How Abutment Design Changes the Decision
Abutment design plays a major role in cement-retained restorations because the crown depends on the abutment for:
- margin position,
- emergence profile,
- retention form,
- path of insertion,
- tissue support,
- cement cleanup access.
A poorly designed abutment can make a cement-retained restoration much more difficult to manage. A well-designed custom abutment can improve margin accessibility and reduce restorative compromise.
In screw-retained restorations, the role of the abutment may differ depending on whether the crown is directly screw-retained or supported by a screw-retained abutment. Either way, the restorative geometry is still strongly shaped by implant position and design choices.
This is one reason why retention planning and abutment planning should always be discussed together.
Esthetics: Where Cement-Retained Can Still Win
The main esthetic argument for cement-retained restorations is simple: there is no visible screw access hole through the crown.
In some cases, this matters a great deal. If the screw channel would emerge through a visible or functionally awkward part of the restoration, the esthetic result may suffer. Even if the access is restored well, it may still introduce a compromise compared with a crown surface that has no access opening at all.
Cement-retained restorations may therefore offer an esthetic advantage in:
- anterior single-unit restorations,
- cases with visible incisal edges,
- cases where facial access would be unacceptable,
- situations where implant angle cannot be corrected sufficiently.
That said, modern restorative techniques and angulated screw channel systems have reduced this difference in some cases. So the esthetic advantage of cement retention should be evaluated in the context of the actual case rather than assumed automatically.
Maintenance and Long-Term Service
Long-term maintenance is often where screw-retained restorations show their strongest practical advantage.
Over time, implant restorations may need:
- screw retightening,
- crown repair,
- hygiene intervention,
- modification,
- replacement,
- inspection of underlying components.
A screw-retained design usually makes these interventions easier and more controlled.
Cement-retained restorations may still perform very well, but when future access is needed, they are often less convenient. In some cases, removal can be unpredictable or destructive, especially if the restoration was not designed with retrievability in mind.
This is why many clinicians increasingly favor screw-retained solutions whenever case conditions make them possible.
Screw-Retained vs Cement-Retained in Anterior Cases
Anterior implant restorations are often the most difficult because both esthetics and tissue behavior matter so much.
In these cases, screw-retained restorations are attractive if:
- the access channel is favorably positioned,
- implant angle is ideal,
- tissue conditions are supportive,
- retrievability is desired without esthetic compromise.
Cement-retained restorations are attractive if:
- screw access would be too visible,
- implant angle is less favorable,
- a custom abutment can place margins appropriately,
- the restorative team prioritizes a more natural visible crown surface.
The correct answer often depends on balancing esthetics with biologic and maintenance realities. This is where careful implant planning and lab communication make the biggest difference.
Screw-Retained vs Cement-Retained in Posterior Cases
Posterior cases often shift the decision toward function, access, and maintenance rather than appearance.
Because the screw access channel is often less esthetically problematic in posterior teeth, screw-retained restorations may become the preferred solution more often in these areas. They offer retrievability and eliminate cement risk, both of which are valuable under functional conditions.
Cement-retained posterior restorations can still work well, especially when implant position and margin access are favorable. But the practical advantages of screw retention often become stronger when esthetic pressure is lower.
How Digital Workflow Changes the Decision
Digital planning has improved both approaches, but it has also made case selection more precise.
With modern digital workflow, the clinic and lab can evaluate:
- implant angle,
- screw access path,
- tissue contour,
- crown form,
- restorative space,
- margin position,
- esthetic consequences,
- retrievability needs.
This makes it easier to choose the retention strategy intentionally rather than by default. The decision becomes more restorative-driven and more specific to the actual implant position.
In advanced workflows, this also allows better coordination between:
- implant placement,
- abutment design,
- retention strategy,
- restorative shape,
- long-term maintenance planning.
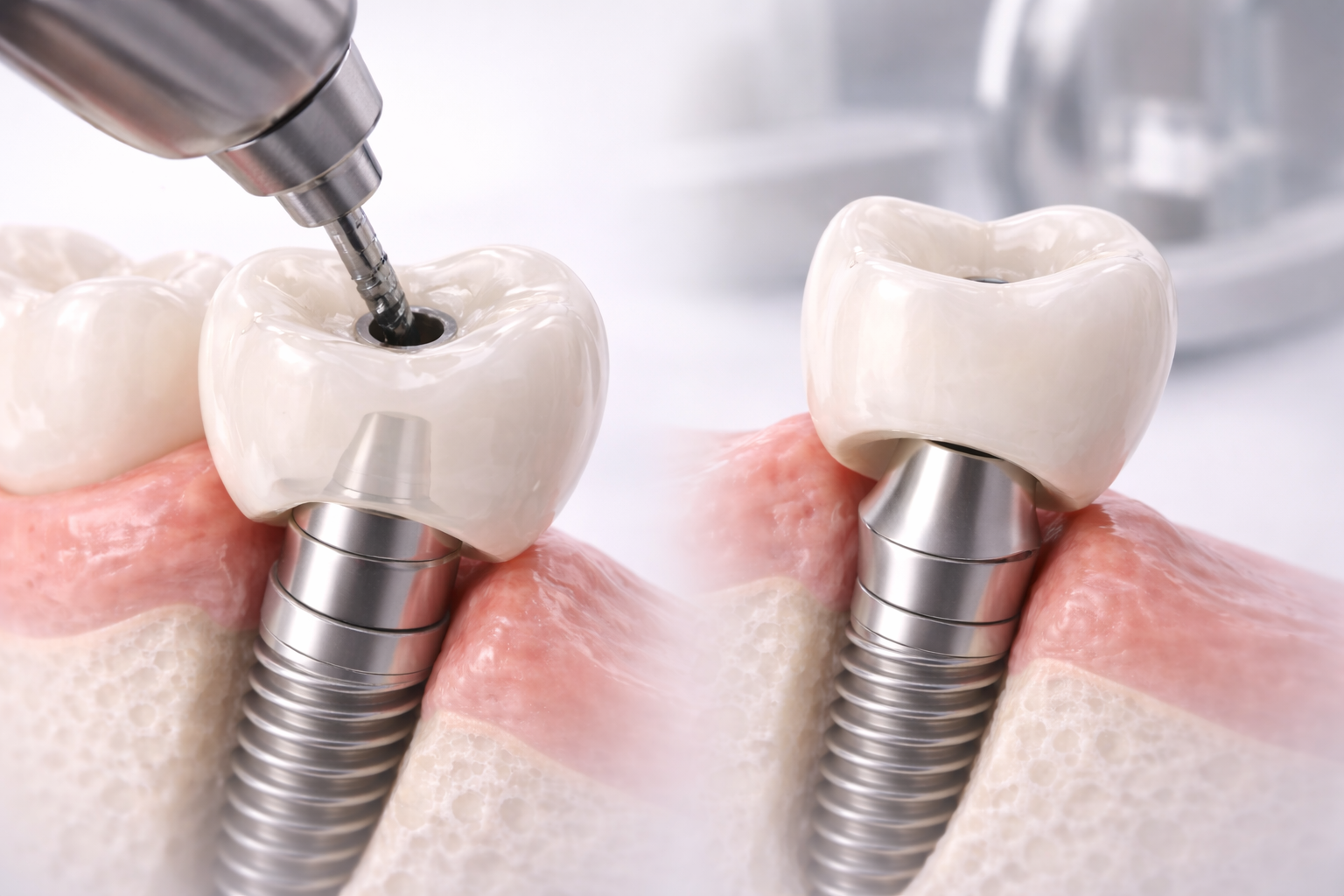
Common Mistakes in Retention Planning
A common mistake is choosing cement-retained restoration in a case where margins will be too deep for reliable cement cleanup. Even if the crown looks excellent at delivery, that choice may create biologic risk later.
Another common mistake is choosing screw-retained restoration in a case where the screw access path creates obvious esthetic compromise and the team has not planned properly for it.
Other frequent mistakes include:
- ignoring implant angulation,
- separating retention planning from abutment planning,
- focusing only on appearance and not serviceability,
- using the same retention approach in every case out of habit,
- underestimating future maintenance needs.
The best retention choice is not the one that wins every theoretical debate. It is the one that fits the real case best.
A Practical Way to Think About the Decision
A useful starting question is this: what matters more in this case—retrievability or esthetic surface control?
If retrievability, maintenance, and biologic risk reduction dominate the case, screw-retained restoration often makes more sense.
If implant angulation creates esthetic limitations and a well-managed cement-retained design can solve them without creating deep-margin problems, cement retention may be the better option.
Then evaluate:
- implant angle,
- tissue visibility,
- anterior vs posterior location,
- smile line,
- margin accessibility,
- restorative space,
- maintenance expectations,
- abutment design quality.
The right answer is usually case-specific. In challenging cases, soft tissue outcomes can be improved using custom healing abutments.
Conclusion
Screw-retained and cement-retained implant restorations can both work successfully, but they are not equivalent in every case.
Screw-retained restorations often offer stronger advantages in retrievability, maintenance, and cement-risk avoidance. Cement-retained restorations may offer esthetic advantages when implant angulation makes screw access less ideal and when margin design can still be managed properly.
The best choice depends on the full restorative context: implant position, esthetic demands, tissue conditions, abutment design, and long-term service expectations. The more carefully that context is evaluated, the more predictable the final result becomes.
FAQ
What is the main advantage of screw-retained implant restorations?
The main advantage is retrievability. Screw-retained restorations are usually easier to remove for maintenance, repair, inspection, and future restorative intervention.
What is the main risk of cement-retained implant restorations?
The main risk is excess cement left around the implant, especially when margins are too deep and difficult to clean thoroughly.
Are screw-retained restorations always better?
No. They are often preferred for maintenance reasons, but in some esthetic cases implant angulation may make cement-retained restoration more practical.
When does cement-retained restoration make the most sense?
It often makes sense when screw access would emerge in an esthetically unacceptable location and when margin access can still be managed safely.
Does implant angulation affect the choice between screw-retained and cement-retained?
Yes. Implant angulation is one of the most important factors because it affects where the screw channel would emerge and how the final crown will look.
Should retention choice be discussed together with abutment design?
Yes. Retention planning and abutment planning are closely connected because both affect margins, contour, esthetics, and maintenance.

